Tucked away on the sixth floor of Teachers College’s Thorndike Hall, the Dean Hope Center for Educational and Psychological Services does not announce its presence to the world.
Yet to those familiar with the Center’s work, there may not be a stronger symbol of TC’s core philosophies, both as a neighbor to its surrounding communities and as an institution that educates with a social justice mission.
Dean Hope serves hundreds of low-income, minority patients in Harlem, Washington Heights and other neighboring areas, who receive affordable individual and group psychotherapy and other services from student trainees. For those who come from cultures in which therapy is often stigmatized — including military veterans, who constitute a significant percentage of Dean Hope clients — the Center makes treatment palatable by offering appointments on a college campus rather than at a readily identifiable medical facility.
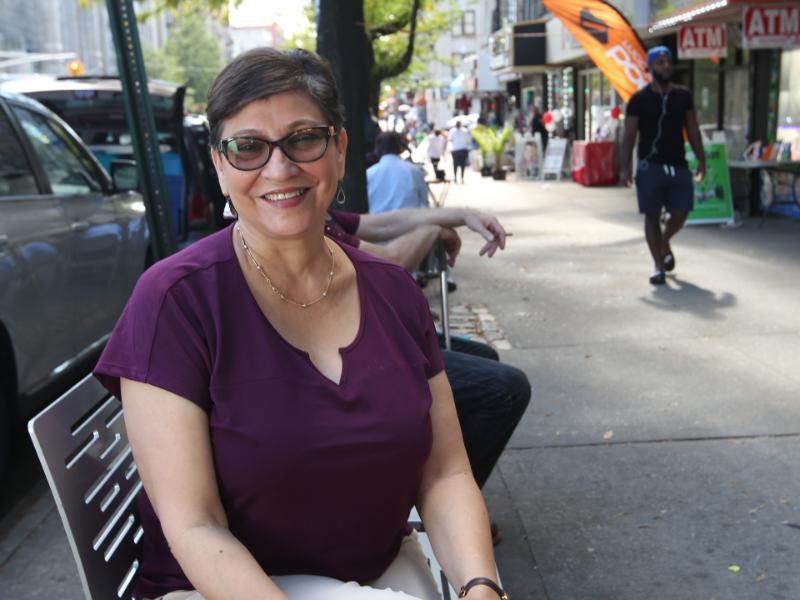
MEETING THE NEED Rosa almost single-handedly moved Dean Hope's operations online and has reduced or waived fees for many patients. (Photo: TC Archives)
“Universities are often perceived by communities as changing the landscape of their neighborhoods without giving anything in return, but our center shows how TC is giving back to our surrounding communities,” says Dinelia Rosa, Dean Hope’s Director.
[Click here to help support the Dean Hope Center’s efforts to continue providing low-cost therapy to patients in need during the COVID pandemic]
Dean Hope is also a critical way station for the students in the College’s Department of Counseling & Clinical Psychology.
“Our entire training during students’ earliest years takes place at Dean Hope,” says Melanie Brewster, Associate Professor of Counseling Psychology, who directs TC’s Counseling Psychology program. “For most, it’s the site where they cut their teeth as therapists.”
It was those considerations that — back in March, when many other counseling and therapy clinics nationwide were shutting down in response to the coronavirus — prompted Rosa to move a portion of Dean Hope’s operations online, taking advantage of the temporary easing of state and federal restrictions on telehealth. No new patients would be added, and the clinic’s testing and evaluation services for children, which must be conducted face-to-face, would remain suspended, but student trainees would be able to resume treating existing patients.
Universities are often perceived by communities as changing the landscape of their neighborhoods without giving anything in return, but our center shows how TC is giving back to our surrounding communities.
—Dinelia Rosa, Dean Hope Center Director
“Our goal was to enable students to continue seeing their ongoing cases through telehealth without interruptions,” Rosa says. “Simultaneously, we were teaching students how to adapt during times of crises.”
Going virtual was not an uncontroversial move. There were concerns about protecting patients’ confidentiality; about the quality of sessions (for the therapists-in-training as well as for the patients); about excluding patients who didn’t own computers; and even about how billing would work (Dean Hope had no access to many of its files).
Eventually, in consultation with professional organizations and legal counsel, the Dean Hope Center addressed these concerns. But ultimately, need was the deciding factor.

BY ALL MEANS In a world in crisis, Verdeli believes online therapy is essential. (Photo: TC Archives)
“Mental health has been a top priority from the beginning of this disaster, which is something you don’t typically see,” says Lena Verdeli, Associate Professor of Psychology & Education, who directs the Clinical Psychology program as well as TC’s Global Mental Health Lab. “In other crises, the focus is usually on providing food, shelter and medication. But because of the need for social distancing, we’re hearing from people who are suffering heartbreak and guilt because they weren’t there to hold loved ones’ hands during their last moments, or to engage in the rituals that would normally follow, or to have the support of the community. People are losing jobs and experiencing changes in their living situations that often force them to spend more time with one another under tighter circumstances — and we know that overcrowding is one of the most stressful conditions for all animals, including humans. So if we have the tools to help, we have to use them.” [Read a story on Verdeli’s views about helping people cope during the pandemic.]
In an era of climate change, pandemics, state fragility, and widespread displacement of populations, e- and m-health [electronic and mobile health] make provision of mental health care possible.
—Lena Verdeli, Associate Professor of Psychology & Education
To put it in psychological terms, an adaptive response was in order.
“This kind of situation creates a shift of mindset,” says Vijayeta Sinh (Ph.D. ’11), a New York City therapist and TC alumna who is part of a network of clinicians who supervise students at Dean Hope. “Before, we did it one way, because that’s how it was always done. Now there’s more flexibility, in part because there’s no choice.”
Dean Hope’s flexibility owes to two key assets. The first is TC’s pre-COVID investment in the online platform Zoom, which has enabled the College to carry on its business on many levels — including moving nearly 800 courses online in the middle of the spring semester.
“I have to say that, checking with other clinics, we are blessed,” Rosa says. “We’ve gotten incredible institutional support, from our operating budget to the infrastructure created by TCIT [Teachers College Information Technology].”
The second critical factor has been the director herself.
During an intense 10-day period over the College’s spring break, Rosa contacted the New York State Education Department, the American Psychological Association (APA) and several other organizations, and also consulted with a lawyer, to create guidelines for all students conducting online therapy. She procured four training modules offered by the APA and made sure that all students watched them. She worked with the TC general counsel’s office to adapt an APA telehealth patient consent form and make it functional for remote use through a program called Adobe Sign. And she contacted Sinh and others in the College’s network of clinical supervisors to make sure they were still willing to offer supervision online.
“Dinelia moved a whole service from in-person to online in a week,” says Verdeli. “She was in close communication with the program directors, often several times a day, to build consensus around our new procedures. She did an amazing job.”
“It’s been very important for Dean Hope to continue its work,” Brewster adds. “Everyone from Dinelia on down has done the best they could in rapidly evolving circumstances, and students and supervisors have been willing to go with the flow. I’ve been very impressed by that.”
“I’m type A, and this is how I manage my own anxiety,” Rosa says with a laugh. “Seriously, though, one thing I’ve learned in my career is to stay connected with professional organizations such as the APA and the New York State Psychological Association. [Rosa is a past president of both the latter organization and the New York Association of Hispanic Mental Health Professionals.] “It’s been so helpful to me now, because I’m able to pull from these different resources.”
[Read a story about Dinelia Rosa.]
By early April, about 30 TC students were treating more than 150 patients online, and two students were also leading a small group.
TC has never demanded that the Center bring in high revenues from client’s fees, which is not the case at many other institutions. When the crisis hit, I asked if we could lower our fees by 50 percent for people who were losing their jobs, or in some cases even waive the fees entirely. And the College has supported that.
—Dinelia Rosa
But Rosa didn’t stop there. She also won approval from the College to financially accommodate patients who had lost their jobs or were facing layoffs because of COVID.
“TC has never demanded that the Center bring in high revenues from client’s fees, which is not the case at many other institutions,” Rosa says. “When the crisis hit, I asked if we could lower our fees by 50 percent for people who were losing their jobs, or in some cases even waive the fees entirely. And the College has supported that.”
She’s made a point of sensitizing students to those same concerns.
“We are psychologists, but we have to attend to clients’ primary needs. If someone says, ‘I’ve lost my job, I can’t pay my rent, I may lose my apartment’ — we’re not experts but we’ve got to learn how you apply for unemployment and how you access other kinds of services. We really have to keep in mind patients’ concrete needs. I tell my students, it’s not just about feelings — if you’re up on that other stuff, it’s really going to make clients feel supported.”
It’s a critical juncture in the career of any therapist-in-training: the transition from absorbing theory in the classroom to treating actual patients for the first time.

TRIAL BY FIRE Treating patients for the first time is always challenging, but Newman and other students are now adjusting to doing it online. (Courtesy of Mandy Newman)
“At TC, we’re highly supported by supervisors and practicum classes, but ultimately it’s trial by fire,” says third-year Clinical Psychology doctoral student Mandy Newman. “You’re applying theory to the practice of cognitive behavioral therapy, family therapy, psychodynamics, child adolescent therapy. You’re tasked with being creative, but you’re learning as you go along. There are moments when you’re unsure if you’re saying or doing the right thing.”
That was the scenario Newman and her fellow students were facing before they began treating patients online.
Since then, the learning curve has gotten steeper at every level. From the moment a student therapist schedules a session with a patient — a task that clinic administrative staff used to perform, but which students now handle by calling patients from blocked cell phone numbers — the dynamics of sessions are markedly different.
A lot of the work we do as therapists is about being comfortable with silence — holding space for patients’ anxiety and ambivalence. When you’re with them, you can make a point of it by just sitting there and letting something materialize. But over the phone or through Zoom, it’s much less possible to follow through with a more intentional silence...someone’s partner coughs, or there’s just more awkwardness, discomfort and uncertainty from looking at one another on the screen.
—Mandy Newman, third-year Clinical Psychology doctoral student
“It’s harder to focus on Zoom,” Newman says. “People are confined to little boxes onscreen, and if you look away for a second or get distracted, you lose something.”
As a result, connecting with patients emotionally is more difficult.
“The training videos say to be more animated, because it’s harder for people to see your emotionality onscreen. Sometimes the energy it takes to express an emotion is like what an actor has to put out. It’s more than you would do when you’re in a room with someone and they can sense things.”
As with acting, nuances can get lost when you’re trying, metaphorically speaking, to ensure that you’re reaching the people in the back rows.
“It’s tricky because a lot of the work we do as therapists is about being comfortable with silence — holding space for patients’ anxiety and ambivalence. When you’re with them, you can make a point of it by just sitting there and letting something materialize. But over the phone or through Zoom, it’s much less possible to follow through with a more intentional silence because other things happen. Someone’s partner coughs, or there’s just more awkwardness, discomfort and uncertainty from looking at one another on the screen. You’re wondering, does it come from the patient not wanting to speak about something, or is it the result of this novel situation?”
Privacy issues, too, become more paramount, especially for patients whose families may not know they are seeing a therapist.
“Clients often can’t be by themselves in their homes, so they’ll sit outside somewhere, and you hear city noises — skate boards, cars honking, people shouting,” Newman says. “Or if they’re inside, you might hear a family member or partner in the background — or pets. I was doing a session when the client’s five cats pushed through the door. It can be funny, but people feel exposed and they’re not as disinhibited.”
There have been patients who simply can’t adapt to having sessions online, either because of their surrounding circumstances or their own discomfort. When the changeover occurred, Newman and other student trainees were tasked with determining, at the outset, where clients were connecting from, and thereafter with monitoring whether the arrangement was truly workable for the patient. If someone wants to terminate treatment, they have to assess issues such as risk for suicide, and they have to know what other resources, including hospitals, are available to the patient.
But it’s not only the patients who must contend with a sense of exposure.
“As therapists, we’re trained to disclose very little about our own lives, because it might influence the direction of therapy,” Newman says. “The client needs to feel taken care of, not the other way around. But now, because we’re working from home, they might see the art on our walls, or a poster or book in the background, which definitely reveals something about you that would not have been revealed before.”
Perhaps most of all, the shared context of COVID blurs boundaries.
“This situation has brought up uncertainties about our roles. We’re all going through this same experience, and it’s important and even helpful to acknowledge that. I want to be human and relatable and bond with the client over what is going on.”
Teaching and Listening: The Supervisor
One of the hallmarks of the Dean Hope Center is the quality of the supervising therapists — many of whom are TC and Dean Hope alumni — who help students wrestle with such issues.
“These are licensed professionals working out in the community in hospitals or private practice,” Rosa says. “They’re not only highly experienced and skilled, but also deeply committed to our program and our students. Most of them do this on a volunteer basis, for no pay, because they enjoy working with our students. Some have been working with us for 20 years, and God forbid I don’t give them a student each July.”

WEARING MANY HATS Student supervisors such as Sinh are monitoring their own wellbeing in addition to that of students and students’ clients. (Photo courtesy Vijayeta Sinh)
Under normal circumstances, supervisors meet weekly with students and sometimes come to the Dean Hope Center to watch students’ sessions with patients through one-way observation windows. But now, working online and coping with the broader context of the pandemic, they, too, are having to adjust.
For Vijayeta Sinh, who became a Dean Hope supervisor a year ago but has worked in a similar role for several years at Mt. Sinai Roosevelt Hospital, the most obvious change has been that, not surprisingly, anxiety levels are “way up” among patients, students — and supervisors, too.
“We’re all doing things — sanitizing grocery bags, taking shoes off — that we never imagined having to do,” she says. “Everyone is struggling to keep their sanity, and among many people with panic and OCD, those symptoms have skyrocketed. For others, there’s also an element of relief — ‘the world is now experiencing the level of anxiety I always have, so now we’re in this together.’”
Your students are in some ways under your care as well. The patient is still the main responsibility, but the students are the point people. They can’t do their jobs if they’re not emotionally OK.
—Vijayeta Sinh (Ph.D. ’11), New York City therapist and Dean Hope student supervisor
On the one hand, she says, the work for supervisors now includes “monitoring our own health and being aware of how our own stresses are playing out in the treatment. Essentially, it’s that idea of ‘put on your own oxygen mask first’ so that we can be helpful to other people and understand the level of stress they’re facing.”
But at the same time, the pandemic has underscored that “your students are in some ways under your care as well.” Sinh says she starts all supervisory sessions now by asking students how they are holding up, and specifically, how they’re managing the stresses of the pandemic. “The patient is still the main responsibility, but the students are the point people. They can’t do their jobs if they’re not emotionally OK.”
Sinh cites the example of a student trainee who, early on in the pandemic, was grappling with some personal issues that overlapped with those of a patient.
“The patient was thinking of moving back home, but was concerned about jeopardizing the health of a parent with compromised immunity,” Sinh explains. “It was hard for the student trainee, because he, too, was thinking about moving back in with family where there were elderly relatives. Working with this patient was bringing up issues of guilt, unease and regret — ‘should I have gone at an earlier time?’ Supervision can be especially helpful in that regard — a place to say, ‘I’m having a little trouble with my own feelings, how do I sort that out?’ And as a supervisor, I’m being more direct in asking students to think of how they may have been personally impacted as a way of thinking about how real this may be for their clients as well—to use their personal experience as a launching pad to exploring their client’s experience and struggles.”
In May, the Dean Hope Center moved into what Dinelia Rosa terms Phase II of its response to the COVID pandemic. For the first time since moving online, the Center is allowing students to take on new patients, though only those who are dealing with COVID-related anxieties or have been diagnosed with the virus. Rosa has continued to cut fees for those in need, sometimes to as little as $10 per session.
At the same time, Professor of Clinical Psychology Douglas Mennin, developer of Emotional Regulation Therapy (ERT) for generalized anxiety disorder, has launched a trial of an abbreviated form of ERT to help people suffering from elevated rumination, worry and distress related to COVID-19. The study particularly reaches out to individuals from low-income and communities of color, which have been disproportionately hit by COVID-19. It uses a number of TC students to deliver Zoom-screen sessions to participants. [Read a story about Mennin’s study.]
And meanwhile, Rohini Bagrodia, a student with prior experience running a therapy hotline, has been working on launching a similar service for Dean Hope. Two other students, Ann Renaud and Charlotte Pfeffer, are creating an online group for women who have recently rejoined the community after being incarcerated.

GOING WITH THE FLOW Brewster is heartened by how TC's psychology faculty, staff and students have adapted to the crisis. (Photo: TC Archives)
All of these efforts, obviously, respond to the ongoing crisis. But they may also be harbingers of a new normal, in which online psychotherapy is a staple of the field.
“For a number of years in my global mental health projects we have been using mobile and telehealth for training workshops, therapy, supervision, research, and program evaluation, and my experience has been very positive,” says Verdeli, who has worked with refugee populations in Lebanon, Uganda and other nations. “In an era of climate change, pandemics, state fragility, and widespread displacement of populations, e- and m-health [electronic and mobile health] make provision of mental health care possible.”
The most important thing is to have people initiate and continue in therapy. The whole field has had to loosen up because of COVID. And I think we’ll see that the world doesn’t fall apart.
— Melanie Brewster, Associate Professor of Counseling Psychology
Dinelia Rosa believes that the College has an obligation to prepare students for this new environment. “Everything we’ve done at Dean Hope and working in collaboration with our academic programs is aimed at preparing our students to join a workforce that can respond to the new, integrated reality of face-to-face and telehealth work.”
Vijayeta Sinh sees online therapy as an antidote to a hypermobile society.
“In the past, if people moved reached out from across the country, I couldn’t help them. With telehealth, I can. Also, many people find therapists through word of mouth, and networks of personal acquaintances aren’t limited by geography — so this opens up the possibility to explore options that feel safe because other people have validated them.”
Telehealth could also free some therapists from shouldering the cost of office space — in places like New York City, an increasingly prohibitive burden in a time when the profession is being squeezed by decreasing insurance reimbursements.
Melanie Brewster, too, hopes online treatment is here to stay and that the practice will also permanently change training and accreditation.
“The most important thing is to have people initiate and continue in therapy,” she says. “The whole field has had to loosen up because of COVID. And I think we’ll see that the world doesn’t fall apart.”
